Captivating CT – Hematuria case study
An 8-year-old neutered male American Bulldog presented with a 2-week history of hematuria but no change to demeanor and no respiratory changes. It was decided that Computed Tomography (CT) should be performed to assess the bladder mass in more detail using intravenous contrast media.
History and clinical investigations
An 8-year-old neutered male American Bulldog presented with a 2-week history of hematuria but no change to demeanor and no respiratory changes. Routine bloods were completed, and ultrasound of the abdominal and pelvic cavities was performed. This revealed a mass on the ventral bladder wall close to the trigone, and enlarged lymph nodes. It was decided that Computed Tomography (CT) should be performed to assess the bladder mass in more detail using intravenous contrast media. The plan for the CT scan was to image the thorax, abdomen, and pelvis (‘TAP’) before and after contrast media, to assess all vasculature and organs, and to attain more information on the urinary tract. The patient was placed under general anesthesia and apnoea was induced during scan acquisition to reduce movement artefact in the thoracic images.
Computed tomography: Positioning
A 32 slice CT scanner (GE Revolution ACT) was used, and an injector pump was available for contrast media administration. This enabled the CT user to time the acquisition of contrast-enhanced images perfectly. The patient was positioned in sternal recumbency, headfirst, with the front limbs extended cranially away from the thorax to avoid streaking artefacts due to photon starvation in the thoracic images. Once the patient was secured with foam sponges and straps, the patient was centered at the apices of the thorax by altering the table height, and the patient was laterally centered for dose modulation purposes. Scout images were acquired of the entire patient, from cranial to the thoracic inlet to distal to the anus. The scouts are very low dose scans which are performed for scan planning purposes and for allowing automatic dose modulation.
A tip for scanning the bladder is to elevate the pelvis so that the contrast-enhanced urine pools in the cranioventral bladder away from the trigone area. In this patient with a mass identified near the trigone of the bladder it was even more important to do this.
Computed tomography: Protocol
The protocol used was the TAP + C using 1.25mm thick slices with 0.625mm intervals. Reconstruction was performed in lung, bone, and soft tissue window widths (WW) and window levels (WL). Following the induction of apnoea, the thorax was scanned from the base of the lungs going cranially towards the head. The abdomen and pelvis were then scanned from the top of the dome of the liver down past the anus, to include all lymph nodes.
The above scans were then repeated following the administration of intravenous contrast media. The acquisition of contrast-enhanced images is diagnostically important and should be performed unless the patient is urinary system compromised, as indicated by history or hematology/biochemistry, or if the patient has had a previous adverse reaction to contrast media.
Computed tomography: notes on urinary tract scanning
CT is a valuable tool for assessing the urinary system for many conditions, from renal calculi to masses and ruptures. Visualizing the entire urinary system in both pre- and post-contrast images is vital for excluding a wide range of possible pathologies. The pre-contrast phase enables identification of the bladder and both kidneys, and to assess for calcified lesions which could be causing hematuria. Contrast-enhanced urine could mask this pathology.
In the parenchymal phase the contrast enhancement is mostly seen in the renal cortex, including the mucosa and the bladder, followed by the excretory phase where the renal pelvis and ureters are visualised better. This is why we ensure we capture all 3 phases to assess any renal disease. This can vary with each patient, so having a protocol ready to repeat as soon as acquired can make it easier to capture images with correct timings.
Computed tomography: notes on thoracic scanning
When imaging the thorax, it is important to have thin-enough slices to identify any subtle changes in the lung tissue. Equally important is the speed of scan acquisition to capture images when the patient is in induced apnoea. This protocol used 1.25mm slices with 0.625mm intervals, with a 1 second rotation time. This gives an average acquisition time of 19 seconds on an 80kg patient, which is achievable for induced apneoa. The thorax is reconstructed primarily with a lung WW/WL, but soft tissue and bone windows are also done post processing to ensure no pathology is missed. Ideally, the more inflation within the thorax, the more detail shown, and less chance of masked pathology due to collapsed lung fields. Pulmonary carcinomas are common, usually slow-growing masses that cavitate and seed metastases to the lungs and other organs, which makes CT the modality of choice when assessing disease progression.
Diagnosis
There was an approximately 4cm soft tissue mass located in the bladder trigone (Images 1 – 2). The mass dislocated the right ureter abaxially and dorsally, but was not causing obstruction. There was a large, approximately 7cm x 7cm x2cm parietal mass in the cranial wall of the gastric fundus. The mass protruded into the gastric lumen and was accompanied by an alteration of gastric wall layering (Image 3). A smaller mass was identified in the wall of the greater curvature of the stomach, measuring approximately 4cm x 1cm. The cranial abdominal lymph nodes were enlarged and hypoattenuating (Image 4). No other abnormalities were seen.
The pre-contrast images of the thorax showed a large bronchocentric mass in the right caudal lung lobe, with irregular contours (Image 5). There was one further smaller nodule in the periphery of the right caudal lung (Image 6). The cardiovascular, mediastinum and trachea all appeared normal.
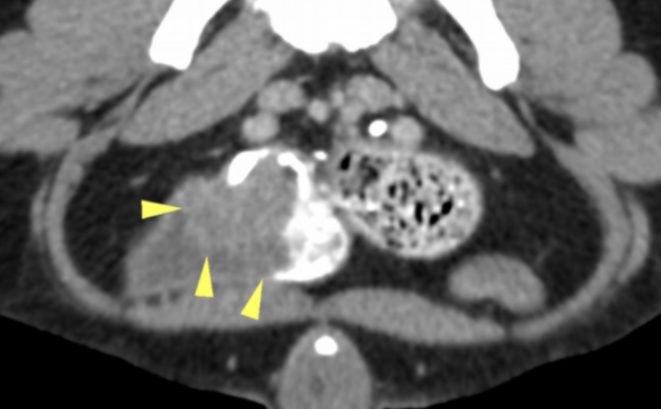
Image 1: Axial slice of a post-contrast scan showing the mass in the bladder trigone (arrowheads).
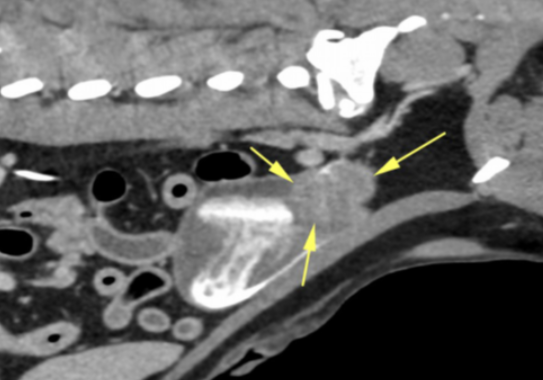
Image 2: Sagittal slice of a post-contrast scan showing a mass in the bladder trigone (arrows).
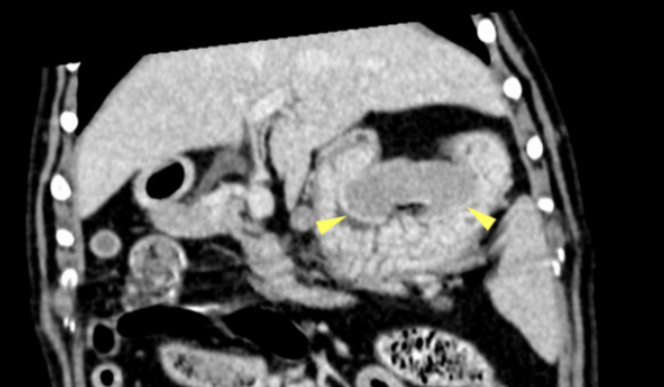
Image 3: Dorsal reconstruction of a post-contrast scan showing a large mass in the gastric fundus (arrowheads).
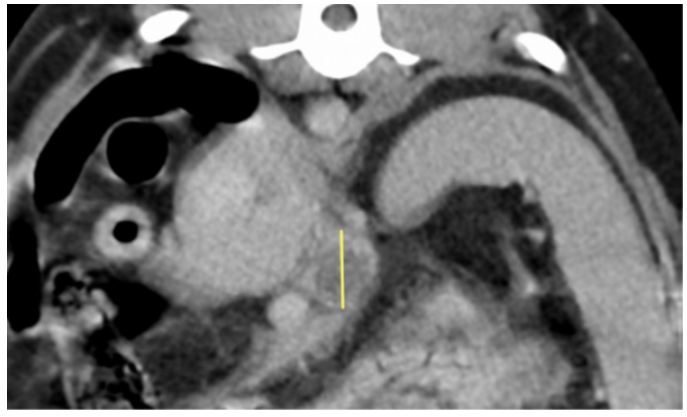
Image 4: Axial slice of a post-contrast scan showing an enlarged left hepatic/portal lymph node with hypoattenuation ( yellow line indicates extent of dorsoventral width).
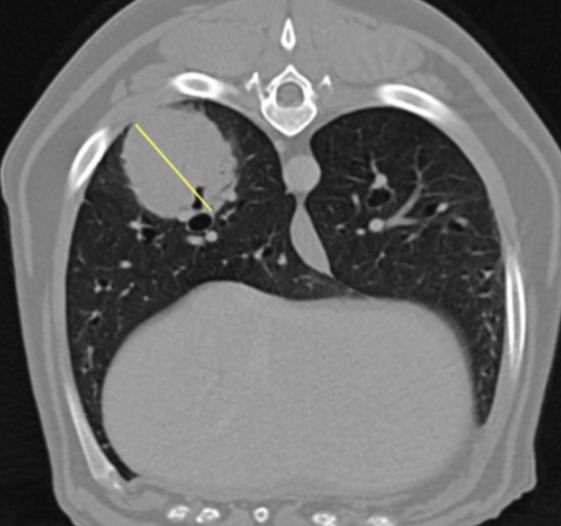
Image 5: Large nodule in the right caudal lung lobe (yellow line indicates width).
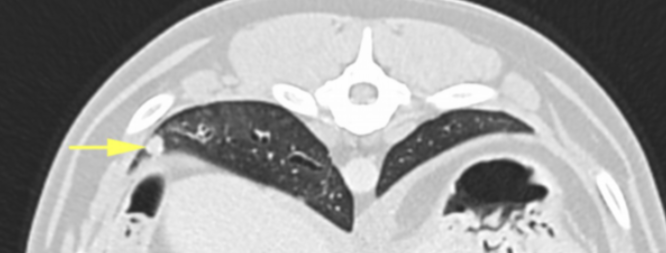
Image 6: Small nodule in the right caudal lung lobe (arrow).
Computed tomography guided biopsy
Once the images were acquired and the patient was stable, it was decided to attempt to biopsy the mass in the right caudal lung lobe, in order to obtain a definitive diagnosis. Identification of the nodule was attempted using ultrasonography; however this was unsuccessful and so CT-guided biopsy was performed.
This procedure is performed routinely within the human world, so a protocol for biopsy was developed from the standard thorax + C protocol. The patient was still under general anesthesia and was stable enough to proceed. By using metal needles as the guide, it’s also a relatively low-dose scan to undertake with a high success rate of getting a sample of tissue without causing excessive tissue injury. The main risk with CT lung biopsies is iatrogenic pneumothorax, but these do self-resolve after the procedure, and a low-dose non-contrast CT scan of the thorax can be performed 24 hours after to check for resolution.
The patient was repositioned in sternal recumbency with the forelimbs extended cranially, therefore ensuring easy access to the area where the mass was located. It was possible to continue in the same examination package, so we repeated the scouts to ensure the patient was completely straight and the scanner could modulate correctly to the new patient position. The measuring tool was then employed, to measure how long the needle had to be to reach the center of the mass, and to accurately assess the required needle angle using axial, sagittal and coronal reconstructions. The distance from skin to centre of lesion was approximately 8cm (Image 7). A length of tape, marked every 1cm by small hypodermic needles, was placed over the right thorax from cranial to caudal. A scan was performed, and this allowed accurate identification of the location for biopsy needle placement (Image 8). Although this can cause artefacts, the mass could still be identified by adjusting WW and WL. The measurement tool can also be used to measure the distance from the spinous processes for more accurate location of the target area.
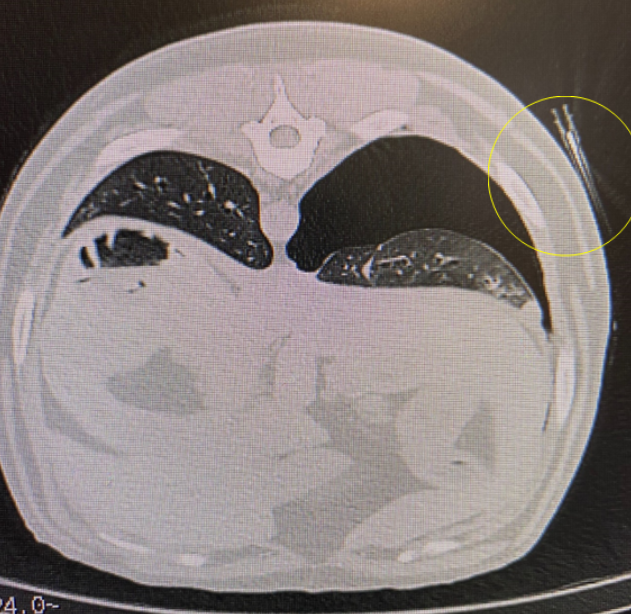
Image 7: Image showing the measurement of distance from the skin to the centre of the mass (yellow arrow).
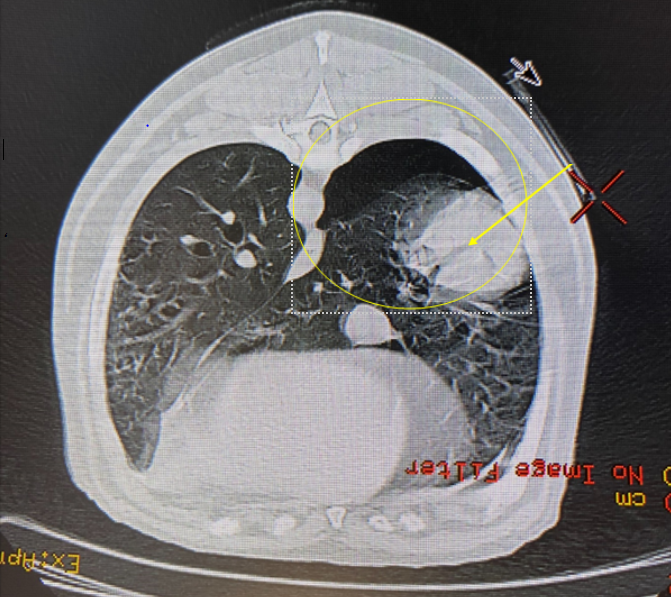
Image 8: Showing the needles placed on the skin to help locate position for biopsy needle placement, relative to the location of the mass.
Once we were happy with the location and the measurement of the length of needle required, we took note of the table position and slice number so we could manually input if we needed to move the patient back to the specific slice. We inserted the 8cm needle and re-scanned the slice position to ensure the needle was correctly located in the mass. We loaded this slice into the reformat viewing platform to ensure the correct location, and then returned to the room and moved the patient out to obtain the samples. After the biopsy samples are acquired, it is protocol to perform another scan through the thorax to check for bleeding and pneumothorax. There was a small iatrogenic pneumothorax present, which would be monitored by rescanning in either 12 or 24 hours and continued clinical observation of the patient. The patient’s pneumothorax was resolved by the next day and he was sent home to await results of the biopsy. Results of the biopsies obtained came back with the confirmed diagnosis of lymphoma.
Conclusion
CT is a very valuable tool when assessing masses. The technology available to us enables us to perform interventional radiology in a way which creates a smooth patient pathway, with minimal invasive procedures, and a one-stop clinic environment.